Over 6 million people in South Africa are currently living with HIV – more
than any other countries in the world. As a middle-income country, South Africa
is in fact doing a lot worse than many other poorer African countries that
suffer from greater shortage of money and health expertise: the HIV adult (aged
15-49) prevalence in SA is approximately 17.8% whereas Uganda has an estimate
of 5.4% and Nigeria has 3.6%. Meanwhile, although South Africa’s HIV epidemic
has grown so large that it affects people from all walks of life, some
populations are significantly more at risk than others. Studies show that HIV
infection in South Africa is distinctly divided along racial lines: 13.6% of
black South Africans are HIV-positive while only 0.3% of whites have the
disease. The epidemic is largely concentrated in black townships and young
black women bear the highest burden of disease. There must be certain reason
why some people are necessarily able to live healthier lives than others. It
seems to me that historical political decisions, notably apartheid, are one of
the major contributors to the current situation.
 | ||
The entrance to the Apartheid Museum in Johannesburg
|
The apartheid legislation in 1949 did not give rise to
the beginning of a new system that creates social inequality, but rather the
conclusion of a long historical development of racial segregation. During the
apartheid era, the society was stratified along racial lines in almost every
aspect of human life, including workplace, schools, residential environments,
civic activity, healthcare, and social intercourse. Although the HIV epidemic,
which emerged in South Africa around 1982, wasn’t widely addressed until a
decade later, the apartheid policies consolidated a variety of distinctive
features of South African history that would account for the prevalence of HIV/AIDS, including racial and gender discrimination, income inequalities, migrant
labor, the destruction of family life, and extreme violence. Since apartheid
was eventually ended at the negotiation table in early 1990s rather than by
revolution, no fundamental restructuring of the socio-economic system occurred,
and many of the inequalities remain and continue to shape the contemporary
landscape of public health in South Africa.
 Starting in 1948, millions of black people were forcibly
removed to Bantustans, areas of land centered on the rural labor reserves,
which comprised of merely 13% of total size of land yet were home to over 80%
of the population. In those areas, health services were largely compromised by
abuse and maltreatment due to poor funding and regulation by the national
government. In 1978, for example, only 0.23% of the South African GNP was
allocated to health systems in Bantustans whereas as 2.3% was given to urban
health centers. Also, in early 1970s, doctor to population ratio was estimated
at 1:15 000 compared with 1:1700 in the rest of the country. As a result,
residents of these under-resourced townships have become extremely vulnerable
to infectious diseases like HIV/AIDS, with little access to quality care.
Starting in 1948, millions of black people were forcibly
removed to Bantustans, areas of land centered on the rural labor reserves,
which comprised of merely 13% of total size of land yet were home to over 80%
of the population. In those areas, health services were largely compromised by
abuse and maltreatment due to poor funding and regulation by the national
government. In 1978, for example, only 0.23% of the South African GNP was
allocated to health systems in Bantustans whereas as 2.3% was given to urban
health centers. Also, in early 1970s, doctor to population ratio was estimated
at 1:15 000 compared with 1:1700 in the rest of the country. As a result,
residents of these under-resourced townships have become extremely vulnerable
to infectious diseases like HIV/AIDS, with little access to quality care.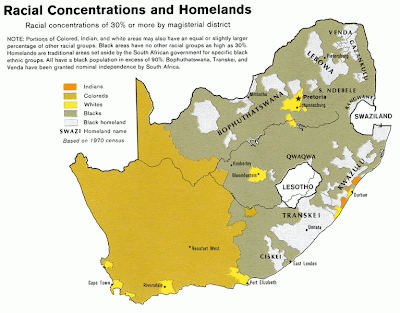 |
| Distribution of black homelands in South Africa during apartheid |
The apartheid government
also adopted a policy of deliberate undereducation of black people, leading to
vast income inequalities in the society, a quarter of the population
unemployed, and overall low educational levels of blacks. These factors in turn
result in greater health inequities, and undermine both the physical and
financial capabilities of blacks in the face of HIV epidemic.
 |
| Several children in a household sharing a bowl of porridge. |
In addition, family life
was extensively destroyed under the migrant labor system, as between
60-80% of the economically active adult men in Bantustans were away from home
to seek jobs while women were dedicated to domestic work. Children were then
increasingly raised by the extended family at home and suffered from high
levels of sexual, physical and emotional abuse and neglect. As a consequence,
both the adults and children are more likely to engage in unsafe &
inconsistent sexual behavior, and become victims of STDs like HIV. Moreover,
persisting gender-based violence, particularly rape and violence against women
in urban areas, further increased the vulnerability of women to HIV/AIDS.
Furthermore, the apartheid era witnessed the beginning of
serious fragmentation of health services, including the separation between
public and private sectors, and the inequitable distribution of resources
between geographical areas and different levels of care. At the time, the government allocated more than half of financial and human resources to the private healthcare
system, which had emerged during the 1980s and were only accessible to 15% of the
population dominated by the urban middle class. Meanwhile within the public
sector, more than 80% of the resources went to hospitals. These situations made
it even more difficult for black South Africans in rural areas to access high
quality health care, and to beat HIV.
In conclusion, the
apartheid era has a significant & lasting political, economic and social
impact on the current HIV epidemic in South Africa, with those still-existing
apartheid ideologies and legacies in the healthcare system. In this sense,
apartheid is not yet over.
By Yutong Zhou, 19 July 2013

2 WEEKS AGO I ENDED NATURAL HERBAL TREATMENT FROM TRADITIONAL HEALER WHO IS IN AFRICAN, I GOT RID OF HPV VIRUS OUT OF MY BODY WITH HIS HERBAL TREATMENT. It SO AMAZING I'M FREE FROM THIS VIRUS FOREVER. YOU CAN REACH HIM ON; DRONOKUNHERBALCURE@GMAIL.COM
ReplyDelete